Karatosis Pilaris
Though not medically concerning, Keratosis Pilaris can cause dryness and itching, impacting your self-confidence. At Brentwood Dermatology, your skin is our priority. If you are struggling with Keratosis Pilaris, schedule an appointment with a trusted Brentwood Dermatology provider for a unique treatment plan catered to the needs of your skin. Start your journey to healthy skin!
Examples of Keratosis pilaris
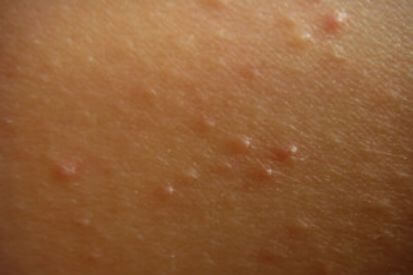
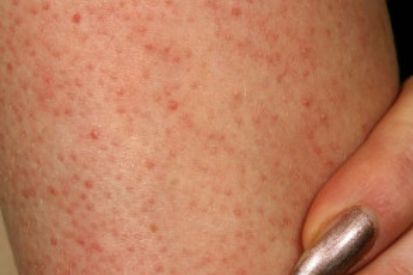
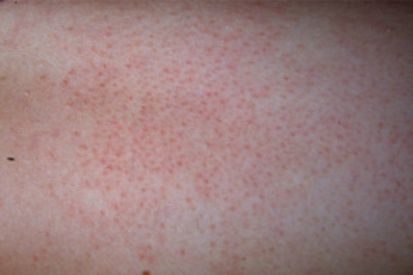

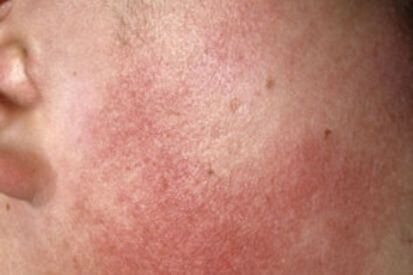
Keratosis Pilaris FAQs
No, keratosis pilaris is not contagious. It is a genetic skin condition that often runs in families. While it may be more common in individuals with dry skin, it is not caused by an infection and cannot be spread to others through contact.
Keratosis pilaris is generally not painful but may cause mild itching. Scratching the bumps can lead to irritation and worsen the condition. Dermatologists can recommend moisturizers and gentle exfoliation to alleviate itching.
For some individuals, keratosis pilaris may improve with age. However, it can persist into adulthood. Dermatologists can provide guidance on managing symptoms throughout different life stages.
While there is no cure for keratosis pilaris, effective management can help control symptoms and improve the appearance of the skin. Consistent use of recommended skincare routines and treatments can minimize the visibility of bumps.
Featured Products for Karatosis Pilaris
Check your local office for current stock!
Check your local office for current stock!
